Plantar Fasciitis

Plantar fasciitis is a very common injury that happens within the foot and ankle. It is the most common cause of heel pain. It affects approximately 2 million people a year. It is caused by inflammation of a strong band of tissue, called a ligament, on the bottom of the foot.
While we encourage you to attempt conservative care at home, delayed care will reduce the efficacy of conservative care. Do not continue to suffer from heel pain, call today to schedule your consultation to meet with a foot and ankle specialist at Central Florida Bone and Joint Institute.
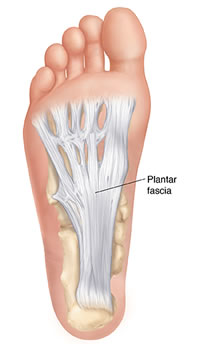
What is the plantar fascia?
What causes plantar fasciitis?
What are the Signs and Symptoms of plantar fasciitis?
How is plantar fasciitis diagnosed?
What are Common Treatments for plantar fasciitis?
What are the surgical treatments for Plantar Fasciitis?
**Disclaimer: Treatment recommendations may vary depending on your true diagnosis. Always follow the recommendations of your orthopedic provider.